Article last updated: March 30, 2021
Surgery’s earliest known document describing the care of wounds, The Edwin Smith Surgical Papyrus, is dated about 1700 B.C. It describes the treatment of difficult wounds encountered on the battlefields of Egypt.
The most widely used and most dependable medicine of that time, honey and grease, was packed into the wound with muslin.
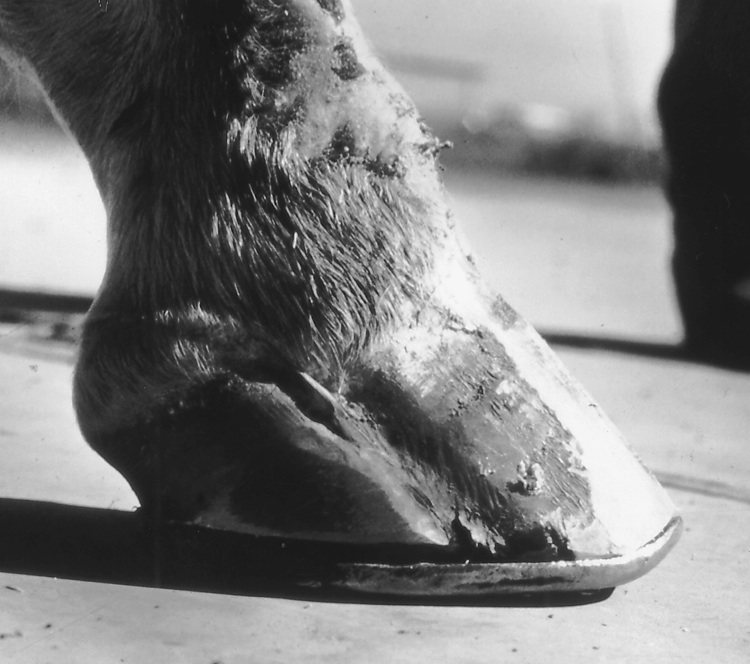
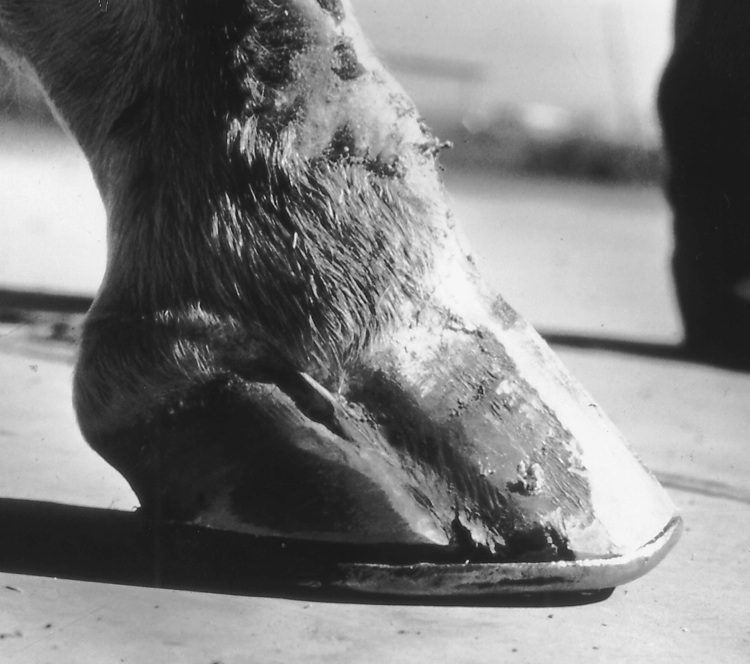
Some 14 days after this hoof was injured, note the lateral wing of P3 and the severe damage that occurred to the extensor tendon.
Substances such as honey, molasses and syrup have been used since ancient time on burns and wounds with a high degree of success. In the 1980s, scientific studies on various sugars used in wound treatment backed up the folklore and ancient medical theories with scientific data (see the updated list of references that accompanies this article).
In the past, extensive research has gone into the use of a mixture of sugar and povidone-iodine in human medicine. Granulated white sugar and a generic ointment commonly called betadine, are mixed into a thick paste with the consistency of toothpaste or peanut butter and applied to the open wound. The starting mixture is roughly nine parts sugar and one part betadine scrub or povidone ointment.
One study was done over a 5-year period in which 605 human patients were treated exclusively with sugardine. In nearly all of these cases, the patients (whose injuries included ulcers, cat scratches and gunshot wounds) healed more rapidly with sugardine than with any alternative method of treatment.
Wound Treatments Left Behind
While surgical techniques have made giant strides during the past century, treatments of wounds themselves have made much slower progress. Some antibiotics are good bactericides, yet are incompatible with infantile tissue.
Antibiotics are generally considered as an injectable medication, while sugardine is commonly used for external treatment.
Knutson et al. said in a 1987 Southern Medical Journal article: “Wounds treated with sugardine differ from wounds treated with antibiotics. Sugar is not an antibiotic by definition, nor when used in connection with povidone-iodine. Unlike those treated with antibiotics, sugardine-treated wounds clean up rapidly; sugardine reduces edema, nourishes the surface cells and has no fetid odor.

A Glu-Strider bar shoe configuration was applied to take all of the weight off the lateral hoof wall and to properly transfer this weight onto the frog.
“The use of sugardine treatment seems to accelerate granulation tissue and epithelial tissue production, thereby covering the wound, burn or ulcer with skin.”
First Sugardine Usage
My introduction to sugardine came in July 1984 from Rich Boronow, M.D., and his wife Gretchen, a nurse and horse owner from Mississippi.
Gretchen owned a magnificent Arabian mare, Fadjesty, which had severe founder and decubitus ulcers. When treating the open wounds of the feet, the irritated soles and hooves were smeared with sugardine, and then bandaged for protection from unhygienic conditions. (Note: All the work described in this article was done under the auspices of or in conjunction with a veterinarian.)
Only after conversations with Boronow and Clyde Copeland, an orthopedic practitioner and my own research, did we begin using sugardine on a regular basis. Some of my early case studies were on horses with exposed phalanges.
One case involved looking at a 14-day old non-weight bearing wound injury on a horse that had a serious laceration with exposed second and third phalanges. Prior to my observation, the wound was initially treated with neomycin powder wraps and antibiotics.
Upon examination, we immediately applied sugardine to the exposed bones with follow-up instructions for 12 days of cleaning and rebandaging. I observed significant improvement after 2 weeks. Within 3 to 4 months, the foot no longer required bandaging and was showing excellent recovery. I attribute the success with this case to sugardine.

The injury was successfully treated 42 days following the first application of sugardine.
Helps Other Wounds
Other instances for using sugardine include canker and severe abscesses. Of these, canker was the only one that failed to improve for me. The severe abscesses, which previously had been treated with 7% iodine or other sometimes-caustic remedies, showed extraordinary improvement and results with the application of sugardine. We also found it effective for dealing with coronary band laceration burns, thrush and decubitus ulcers.
The purulent decubitus ulcers that had occurred with the Mississippi horse were not healing until packed with sugardine. Within 72 hours, healthy granulation was observed and most drainage stopped. Former treatment had been ointments or applications of nitrofurazone, gentian violet or other over-the-counter remedies.
When I analyzed the routine success of sugardine therapy, it far surpassed any former treatment. Therefore, I suggested its usage to many of my farrier and veterinarian colleagues.
Individuals who followed my recommendation called and sent letters regarding their responses and findings. Other sources in different sectors of the country reported 100% recovery in less than 14 days for thrush cases treated with sugardine. These cases were bandaged daily or every other day, depending on the severity of the condition.
However, horses which had a recurrence of the problem did so because of contaminated and unhygenic environments. This research and information only substantiated my initial observations.
An Update On Sugardine
In the past 10 years, there have been several published and peer-reviewed veterinary and human medical articles referencing sugardine for wound management. These have been added to the original list of references posted with this article.
While sugardine has not been formally studied in either the veterinary or human field, the articles agree that the mixture is effective for several reasons.
The sugar draws lymph into the wound, nourishing regenerating tissues and preventing bacteria growth. Swelling is reduced, white cells that help clean and debride the wound are attracted and nourished, and a protective layer of protein is formed over the wound. Sugar also deodorizes necrotic wounds.
— Courtney Diehl, DVM, Steamboat Springs, Colo.
Just Seems Too Simple
At first, many people were reluctant to use sugardine because of its simplicity. Some thought any type of successful wound treatment must be complex or costly to be effective. The remarkable use of sugardine is now accepted more frequently by many veterinarians and farriers because of successful results and its economic significance.
The ingredients, sugar and betadine in scrub solution or ointment, can be purchased for a reasonable cost in most local pharmaceutical or veterinary supply stores. Accessibility, acceptability and affordability establish justification for widespread use on minor cuts, burns and open suppurating wounds by the general horse public.
The value of sugardine is acclaimed by farriers and veterinarians who attest to its significance as a major advancement in equine science.
The late Burney Chapman was an American Farriers’ Association Certified Journeyman Farrier and an International Horseshoeing Hall Of Fame member living in Lubbock, Texas. He specialized in working with lame horse problems and was best known for his pioneering work with the use of the heart bar shoe in laminitis treatment.
REFERENCES
Boronow, R., Mississippi Baptist Medical Center, Jackson, MS. Personal interview.
Bose, B., Honey Or Sugar In Treatment Of Infected Wounds? The Lancet, April 24, 1982, 963.
Chirafe, J., Herszage, L.A., Joseph, A., and Kohn, E.S., In Vitro Study Of Bacterial Growth Inhibition In Concentrated Sugar Solutions: Microbiological Basis For The Use Of Sugar In Treating Infected Wounds. Antimicrobial Agents and Chemotherapy, 1983, 766-773.
Chirafe, J., Herszage, L.A., and Scarmato, G., Scientific Basis For Use Of Granulated Sugar In Treatment Of Infected Wounds. The Lancet, March 6, 1982, 560-561.
Copeland, C., Mississippi Baptist Medical Center, Jackson, MS. Personal interview.
Forrest, R.D., Sugar In The Wound. The Lancet, April 10, 1982, 861.
Hanson, R., New Concepts In The Treatment Of Large Avulsion Wounds In The Distal Extremities. Current Concepts in Wound Management, American Association of Equine Practitioners Proceedings, 2006.
Knutson, R., Merbitz, L.A., Creekmore, M.A., and Snipes, H.G. Use Of Sugar And Povidone-Iodine To Enhance Wound Healing: Five Years Experience. Southern Medical Journal, 1981, 1329-1335.
Noda, Y., Saito M., Watanabe, K., Sanagawa, A., Sobajima, Y., Fujii, S., Physicochemical Characterization Of Tretinoin Tocoferil Emulsion And Povidone-Iodine Sugar Ointment Blend Developed For Improved Regulation Of Wound Moisture. Chem Pharm Bulletin, Tokyo. 2013.
Read, R., Soft Tissue Surgery. Emergency Wound Management. The World Small Animal Veterinary Association proceedings, 2006.
Smeak, D., Update on Wound Management: What Is The Scoop On Sugar? 13th European Society of Veterinary Orthopedics and Traumatology. Congress proceedings, 2006.
Related Content
Sugardine — A Stinky, Gooey Mess That Works When Treating Wound Injuries
Sugardine seems too simple to be effective. At least that's what a lot of my horse owner clients say. Learn more about this remarkably safe and effective wound dressing.
How to Make and Use Sugardine for Horse Wound Treatment
Topical treatments containing sugar have been used for wound care for centuries. Read this step-by-step on how to create sugardine.
Vet, Farrier Tackle Tough Abscess Case
A retired barrel racing horse suffers severe bruising and abscesses after pulling its horseshoes.
Effective Strategies for Fighting Infections of the Hoof Capsule
Unlike infections in soft tissue, which typically erupt with dramatic heat, swelling and pain, infectious conditions of the hoof capsule may present more subtly. The farrier is often the professional best placed to first identify and address the early stages of conditions such as thrush, canker and white line disease. The farrier is also uniquely qualified to provide the first line of defense in the prevention of some of these conditions.
Keratoma Case Report: Trail Riding Horse
A team approach and addressing sound shoeing principles help a horse recover from keratoma.







Post a comment
Report Abusive Comment