American Farriers Journal
American Farriers Journal is the “hands-on” magazine for professional farriers, equine veterinarians and horse care product and service buyers.
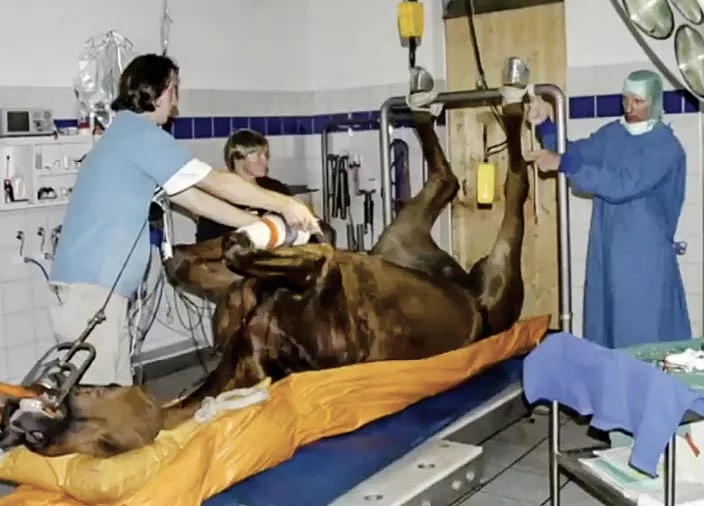
A horse is placed under general anesthesia for colic surgery. Colic can cause systemic inflammatory response system, which may lead to laminitis.

Dr. James Orsini
Laminitis is one of the most dreaded equine diseases. Many horses affected by it eventually develop severe or chronic lameness.
Dr. James Orsini, former director of the Laminitis Institute at the University of Pennsylvania School of Veterinary Medicine’s New Bolton Center, is well-acquainted with the disease. He has seen many laminitic cases as a complication relative to a number of problems. Although laminitis can be successfully treated, it is often a lifelong process that requires considerable time, expense and energy.
Orsini shared his insight about the disease in an American Farriers Journal Online Hoof-Care Classroom webinar “Laminitis: Research and Recommendations on Management for Horse Owners and Horse Care Professionals,” sponsored by Ice Horse.
Understanding the causes of laminitis, Orsini says, helps farriers to prevent and detect early signs to keep the disease from escalating.
The causes of laminitis usually can be broken down into three major etiologies, Orsini says. The one that creates the most devastation to the foot is systemic inflammatory response…