The Connemara Pony is an athletic, versatile equine with a kind and willing temperament. The breed is elegant, hardy and intelligent. A good example should show great agility and superb jumping scope. These attributes have made it one of the most popular United Kingdom native breeds.
However, there is a serious genetic condition that can present in the breed. Hoof Wall Separation Disease (HWSD) affects the bond within the hoof wall. The affected animals present with broken and delaminated feet, which struggle to hold shoes or maintain soundness. It is a serious issue and steps are now being taken to screen breeding animals so that the disease does not become more widespread.
Farrier Takeaways
- Hoof Wall Separation Disease is a genetic condition present with Connemara Ponies.
- There is no cure for this disease; it can only be managed by footcare and owner compliance in the animal’s care.
- There are many factors that will influence your shoe/boot selection.
Explaining The Genetic Condition
HWSD is an autosomal recessive genetic disorder resulting from a single gene mutation. This means that there is a permanent alteration in the DNA sequence of the animal (Finno, 2015).
This mutated gene can be passed onto the offspring regardless of the gender of the parent or offspring (autosomal). The fact it is a recessive gene means that symptoms will only present, if, the offspring inherits the mutated gene from both parents. A pony may be a carrier, with only one copy of the mutated gene. A carrier may be completely sound and will not show any signs of the disease. It is not an acquired condition, and it is incurable.
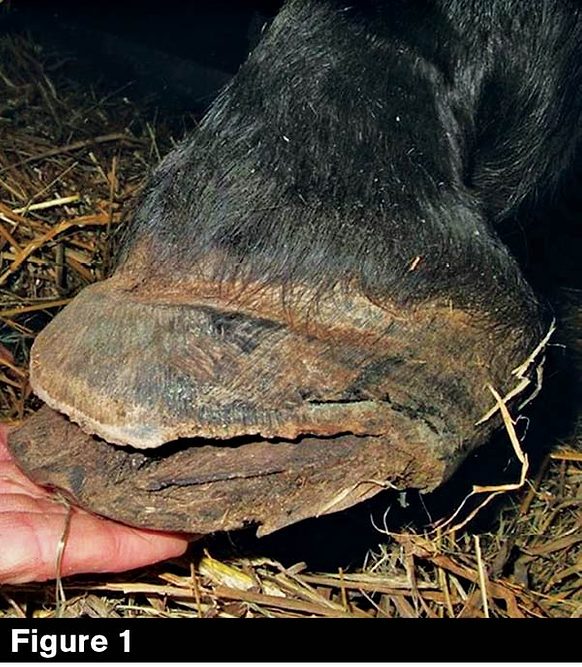
HWSD is characterized by the delamination and separation of the dorsal hoof wall. (Figure 1 above). The bond between the stratum externum and stratum medium fails, causing it to crack and break away easily. The failure in the bond is caused by a malfunction in the lipid metabolism in the extracellular matrix of the hoof wall. In simple terms, there is a lack of “waterproof glue” holding the hoof wall tubules together. Remaining wall may have a “stringy” appearance, in which the intertubular horn has disintegrated, leaving the tubular horn visible.
The signs of deterioration begin to show in young animals — generally between 1 and 6 months of age (Figure 2). The deterioration rate would be affected by many different factors. For example, a young animal in a good environment may appear to have a slower deterioration than one kept in a wet, poor environment. The condition affects all four feet.

Signs of separation start to show in young animals.
In severe cases, the wall disintegrates to the extent that the ponies’ weight is entirely on the sole of the foot. This can lead to severe lameness, abscesses and laminitis.
Shoe loss is a problem with nails tearing out of the poor horn. Some animals may develop large solar callouses, which allow them to cope as grazing animals barefoot but are unlikely to stay sound with use. If a Connemara is showing the signs of HWSD, then genetic testing can confirm whether it has the genetic problem, or if there is another cause for poor horn quality. Common misdiagnosis is type 2, (systemic) seedy toe but this is a bacterial and fungal infection and not a genetic problem.
Disease Management
Good hoof hygiene, diet and management will improve seedy toe, but it will not resolve HWSD. Management of affected ponies involves controlling their living conditions, as extremes of environment or sudden changes can cause rapid deterioration. Dietary supplementation can ensure that no deficiency is present to worsen the horn quality. Skilled farriery can help manage animals with milder symptoms. The use of glue-on shoes and modern materials can be used to reduce the load on the hoof wall and spread the load on the solar surface of the sole and frog (Figure 3).

Glue-on shoes can be used to redistribute load on the solar surface and to lessen the pull on the wall.
The farrier may be unaware that the animal was suffering from the disease — often in non-breeding animals — its only once the feet have disintegrated that desperation makes folks test them. This is still a relatively unknown condition, so there are plenty of animals out there that are just thought to have “poor feet” that may be HWSD. If the animal is known to have HWSD, then I would always shoe and encourage management to preserve the feet in the best way for the individual.
If I had a new horse that I was suspicious of HWSD, then I would push to test it. In that case, the knowledge may allow me to convince the owner that glue-on shoes would be the best way to go as a conservative measure. But often without the test, I have just carried on shoeing as I would “normally” and as appropriate for that horse, which may be glue-ons or fewer nails.
Scheduling the horse tends to mean finding the sweet spot which is maximum growth prior to shoe loss — which doesn’t tend to be very long! A couple of cases that I’ve dealt with (prior to the condition being proved) we used to visit every 4.5 weeks (usual for my area is 6 to 8 weeks).
Careful trimming and the use of boots may suit some affected individuals and allow them to work. Any form of permanently fixed shoe will rely on the hoof wall to some extent, and success of any fixing will depend on the extent of the condition. The principles of good foot balance and functional biomechanics should apply no matter what sort of shoe or boot is applied.
I think the type of shoe comes down to personal preference. My decision will be influenced by the feet, the management (i.e. will the owner do exactly as instructed regarding turnout, feed, exercise, etc). Turnout conditions are important — if they only have a wet field, then there is no point applying methods that do not cope with moisture.
Other conditions to consider for shoeing include the work the owner hopes to do with the animal and also the cost involved. If an owner cannot afford to follow a particular shoeing protocol, then they will try to stretch the shoeings in an attempt to save money before they realize the consequences or before they say they cannot afford the work. A long, honest discussion is always needed before work starts on these horses (diagnosed or not).
Exercise will depend on the animal. The breed can have some quite big variations in type. The surface is important — tarmac and hard ground will put more shock into the hoof wall, whereas a soft turf or arena surface helps absorb some of the shock. Depending on what and where the rider has access to would again influence the shoeing: can I help absorb shock by using different materials? Or should I try to protect the hoof wall from abrasive surfaces? Etc.
None of this can cure HWSD but it might lessen the symptoms and keep the affected pony in comfortable condition.
HWSD has varying degrees of severity, with some ponies being able to stay in work, whilst others due to continuous lameness require euthanasia.
Genetic Testing
The genetic test for HWSD has been available commercially since 2014. It is important that carriers are not excluded from breeding, with a wide spread of the mutated gene within a relatively limited gene pool, exclusion will only further contract the gene pool and potentially cause appearance of other damaging traits. The sole purpose of testing is only to avoid crossing carriers that could result in affected foals being born.
The Connemara Pony Breeders’ Society (CPBS) strongly encourages breeders to undertake voluntary testing of mares and stallions not included in the compulsory testing. From 2016 CPBS has implemented compulsory testing of colts presented for inspections and all registered foals with the results of the test stamped in their passports (CPBS, 2016). Although this is not a commonly known about the disease, education should be encouraged to ensure careful breeding and appropriate management reduce the spread of the disease.
References
- CPBS, 2016. Connemara Pony Breeders Society. Available at cpbs.ie [Accessed 20 April 2017].
- Finno, C. S., 2015. SERPINB11 Frameshift Variant Associated. PloS Genet, 11(4), p. e1005122.
- Finno, C. S. B., 2016. veterinary genetics laboratory UCDavis veterinary medicine. Available atvgl.ucdavis.edu/bannasch/HoofWall
Separation.php [Accessed 20 April 2017].








Post a comment
Report Abusive Comment